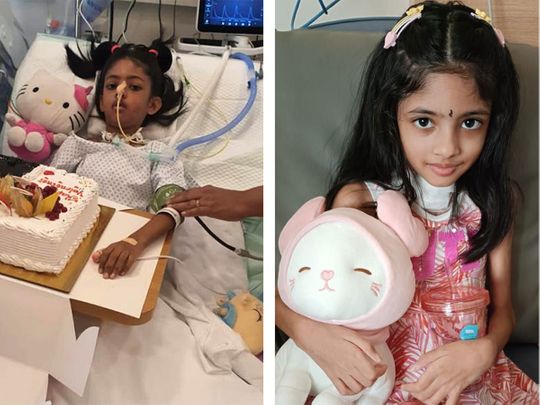
Dubai: When little Surabhi, a Grade 1 student in Dubai, felt weak and listless in January this year, her family put it down to a lot of running around. “It didn’t seem alarming, but we took her to a nearby clinic anyway. The doctors too found nothing amiss,” her father Rajendra Temkar told Gulf News.
However, a couple of days later, Surabhi did not get out of bed. She could not even go to the washroom because she couldn’t get herself to stand or move her legs. Panic-stricken, her parents now rushed her to the emergency department at NMC Royal Hospital DIP. After due investigation, she was diagnosed with what the doctors said was Guillain Barre Syndrome (GBS), a rare neurological disorder.
What followed was a veritable nightmare. The young girl was asked to be shifted to the Pediatric ICU (PICU) at NMC Royal Hospital, Sharjah. “We were told that there was not much time to lose as GBS progresses very fast. In fact, by the time, we reached Sharjah, Surabhi’s condition had worsened and she had to be put on ventilator support,” recalled Temkar.
What is GBS and its symptoms?
According to Dr Deepika Gandhi, Specialist Paediatric Intensivist, who treated Surabhi at the hospital, GBS is a rare neurological disorder in which the patient’s immune system mistakenly starts attacking part of the peripheral nervous system, mainly the nerves outside of the brain and spinal cord.
She said, “Symptoms of GBS can range from very mild involvement of peripheral nerves with brief weakness, to almost complete paralysis of the arms, legs and chest muscles, leading to inability to breathe spontaneously. It can also sometimes affect the patient’s heart rate and blood pressure, and can be life-threatening if not diagnosed in time. Most often, patients present a history of some recent respiratory infection prior to the onset of the muscle weakness.”

She said most often, symptoms of GBS increase in intensity for the first few days, reach a plateau by the second week, and then recover slowly over the next few weeks or months, depending upon the severity and extent of nerve involvement.
In Surabhi’s case, her condition had rapidly worsened due to near-complete paralysis of limb and chest muscles, and she could not even swallow her saliva.
“She was in severe respiratory failure on presentation at our PICU and needed to be put on the ventilator and other life-supportive measures,” the doctor said.
Battling the unknown
Surabhi’s father said, “We had never heard of GBS. We were told she has the acute variant of the syndrome and hence her recovery would be long and slow.”
He said Surabhi was paralysed neck below and her only communication was through her eyes. She couldn’t speak either.

“We would speak and she would respond with her eyes. It took over a month for her to make slight movements of her neck. Surabhi is our first-born and prior to this, she has had no incident of any serious illness. She had a normal birth too. So to see her bedridden, battling a disease we had no clue about for reasons beyond our comprehension was traumatic,” he said.
Dr Gandhi confirmed that Surabhi was in a critical condition with respiratory failure and impending cardio-respiratory arrest when she came to the hospital. “She was stabilised and put on mechanical ventilatory support in view of the respiratory and bulbar paralysis. Her history and clinical signs were suggestive of severe GBS, and she was immediately started on IVIG (specific treatment for management of GBS). MRI brain and spine were normal, but nerve conduction study confirmed acute motor polyneuropathy involving both upper and lower limbs.”
On the ventilator for four months
She said despite the GBS-specific treatment, Surabhi had a long and complicated hospital stay. “She needed tracheostomy for prolonged ventilatory support as she had complete paralysis of all respiratory and bulbar muscles (muscles responsible for swallowing, and preventing choking). With supportive care, a repeat dose of IVIG and intense physiotherapy, her condition began to improve slowly. Despite multiple trials, the ventilator could only be removed after four months, and the tracheostomy two weeks later.”
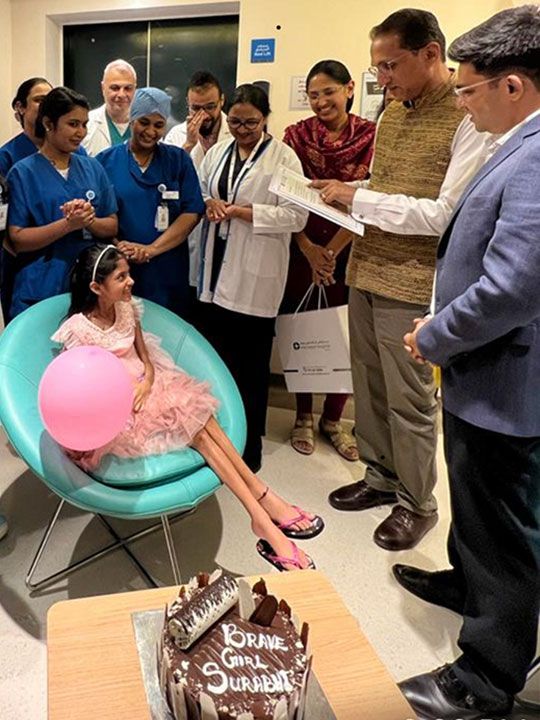
At the time of discharge in June, Surabhi could speak on her own with a normal vocal modulation, was tolerating oral food without choking and her muscle strength had recovered significantly for her to be able to take a few steps with support.
Long and arduous recovery
Dr Gandhi said, “Complete recovery from severe GBS is a long and arduous process. The type of GBS which Surabhi has purely motor nerve involvement and takes months to recover, but most patients are able to achieve normal life and activity by the end of one year. Surabhi has a bright future ahead.”
Temkar said the doctors had prepared the family to face the challenge. “At times like these, keeping your mental health positive is so important and Dr Gandhi provided us that much-needed rationale to keep us going day after day. For us everything was new - this disease, our daughter’s hospitalisation, even Sharjah for that matter as we live in Dubai, but this experience just opened us to an experience of a lifetime.”
He said, “The day they took her off the ventilator was the happiest day alive for us. To see her breathe without any external aid was a blessing. Since the time we have come back home, she has been fine with no issues. She has always loved music and sings and plays when she is in the mood for it. Her two-year-old brother keeps her company.”
School beckons
He said Surabhi missed her last term in Grade 1 due to her hospitalisation. “She has missed her first term in Grade 2 as well. I am hoping she can join the second term. Her assessment clearly indicates that she is okay except for her foot strength, which is creating a bit of a problem for her to stand. But she is undergoing physiotherapy and we hope she will be able to recover fully soon.”










