What to pack in a school lunch box?
School lunch contributes up to one third of a child's daily nutrient intake, so it is essential the items included are healthy and balanced
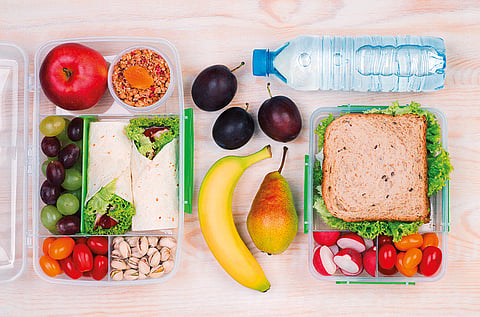
The key to a healthy lunch-box meal is to ensure that it includes items from all of the five food groups.
Dairy (milk/yogurt/cheese) To provide your child with good sources of calcium that is essential for the development of strong, healthy bones.
Fruits Rich in vitamins, minerals, fibre and phytonutrients, which are important for their antioxidant properties.
Cereals Provide energy, aid in digestion and help maintain blood sugar levels.
Lean meat, poultry, fish, nuts and eggs Protein is essential for building, maintaining and repairing tissue.
Vegetables and legumes (beans/peas/lentils) They provide vitamins, minerals, fibre and phytonutrients.
Water Children are at higher risk of dehydration than adults. This is because in relation to their size, children have a greater area of their skin exposed to heat and available for sweat loss. Moreover, children do not always recognise thirst and may forget to drink water if they are not reminded. Children’s water needs are dependent on their age, size and level of activity. On average, children below eight years of age should drink four to six glasses of water. Those older require a minimum of six to eight glasses. Children who are very active, play sports, or have been out on a hot day will require more fluid replacement.
Get your child involved in packing their lunch box. They can help with preparing healthy sandwiches and chopping fruit cubes, as this can reinforce long-term healthy eating habits.
Focus on healthy options for snacks to include in the lunch box and make sure the snacks are neither large enough to affect the main meal, nor small enough to keep the child hungry. Examples of snacks in the lunch box can include home-made popcorn, wholegrain bread topped with peanut butter or low-fat cheese, baby carrots, cucumbers and celery sticks with low-fat cream cheese dip or oil and lemon dip, or some low-fat flavoured yogurt. Avoid adding biscuits, chips or bars in their lunch box in order not to replace the intake of healthy snacks.
Key parts to a healthy lunch box include:
1. Fresh fruit, such as an apple, orange cubes, strawberries and grapes
2. Fresh crunchy vegetables such as baby carrots, cucumber slices and celery sticks
3. Milk, yogurt or cheese (opt for reduced fat for older children). For children who cannot tolerate milk products, you can substitute with fortified soy or rice drink or soy yogurt
4. A meat or meat alternative such as hard-boiled egg, peanut butter or grilled chicken strips
5. A cereal or grain food such as bread, crackers (opt for wholegrain)
6. Water
Tips for healthy lunch boxes:
There should be one portion of fruit and one portion of vegetables or salad every day.
Cut up large pieces of fruit and place them in a container. This will help in making it easier for children to eat.
Cut the sandwich you have prepared in half, one part for first recess and the other for the second. Aim for wholewheat bread in order to help children receive more fibre.
During summer, opt for frozen milk or yogurt to make the snack refreshing for your child. Colour the lunchbox with a variety of vegetables and fruits. This will make it more appealing for the child to eat. Free, fresh drinking water should be available at all times
What to leave out:
1. Sweet drinks such as fruit juices, sports drinks and soft drinks. These are high in calories and in sugar, which can lead to weight gain and oral health issues with children.
2. Dried fruit bars. They are high in sugar, low in fibre and can contribute to tooth decay.
3. Dairy desserts such as chocolate bars as they are usually high in sugar and fat, contributing to weight gain. Confectionery such as chocolate bars, chocolate-coated biscuits and sweets should not be included.
4. Processed meat such as salami and pepperoni. These meats are high in salt and fat.
5. Salted biscuits, nuts and chips
Sample lunchbox:
1. A slow-release energy food: wholegrain or wholemeal carbohydrates.
a. Wholewheat bread, rolls or pita, cooked lentils or chickpeas
2. Growth-aiding foods: Meat, fish, eggs or beans in a sandwich. A hard-boiled egg, tuna in water or slices of low-fat cheese are rich protein sources.
3. Fruits and vegetables: Add a cup of cherries or an apple, vegetable sticks with low-fat dip or some berries in yogurt.
4. Drink: Water bottles are the best choice. To help keep your child hydrated, pack a water bottle in the lunchbox and remind your child to drink water before, during and after any activity. Alternatively, add some milk, smoothies or a yogurt drink.
When packing lunch for children with type 1 or 2 diabetes, the focus should be on healthy options that will help manage their blood glucose levels while keeping them energised throughout the day. Try to avoid high-salt, sugary snacks such as chocolate bars and salted crackers. Opt for fresh fruit, baby carrots and cucumber or wholewheat crackers with a low-fat dip and a low-fat protein source such as cheese, strained yogurt or hummus instead.
Glycaemic index
Particularly important for diabetics, the glycaemic index is a number that gives you an idea about how fast your body converts the carbohydrates in a food into glucose. High glycaemic index foods make your blood sugar shoot up very fast, and this includes refined sugars because they are easier for the body to change into glucose. Low glycaemic index foods, however, are those that are more slowly digested, keeping your sugar levels more steady.
For your child’s lunchbox, replace high glycaemic index foods such as white bread with low glycaemic index foods such as wheat or rye bread. The latter options are high in fibre, vitamins and minerals and will help keep your child fuller for longer. If your child is not a bread fan, you can try replacing it with wholegrain crackers.
Choose a protein filling for the sandwich as it takes longer to digest and will keep your child feeling fuller for longer. Choose leaner meats and low-fat dairies.
Add vegetables such as lettuce, tomato and cucumber to the sandwich.
Include healthy fats such as avocados or low-fat peanut butter as a protein alternative.
Incorporate non-starchy vegetables as snacks in the lunchbox. These can include carrots, cucumbers and broccoli, which can be dipped in low-fat cottage cheese or light dressing.
Add fresh fruits for variety
Replace any packaged sugary fruit yogurts with low-fat yogurt and add your own seeds or fresh berries to it.
For patients with type 1 diabetes, however, it is recommended that a fast source of sugar be available at all times in cases of a hypoglycaemic incident, where blood sugar levels dip below 70mg/dl. Examples of fast sugars includes fresh juice, honey, dates or table sugar.
Most school children are active during recess, so a fast-acting snack should be present in case of hypoglycaemia.
Below are the instructions for the appropriate treatment of hypoglycaemia in diabetc children:
1. When the blood sugar reaches a level under 70mg/dl, 15g of carbohydrates should be consumed in the form of simple sugars. This is equivalent to half a cup of juice, a tablespoon of sugar or honey, or three dates.
2. The blood sugar level should then be checked 10-15 minutes after correction. If it is still below 70mg/dl, then the mode of correction in step number 1 should be repeated.
3. After correction, a snack or main meal should be consumed depending on the following:
a. If the duration until the next main meal is longer than one hour, then a snack consisting of one serving of carbohydrates plus protein should be consumed to prevent a recurrent hypoglycaemic episode.
b. The main meal can be consumed after correction if its timing is less than an hour after the hypoglycaemic episode.


