Dubai woman saved from deadly skin disorder
Jenny Mariano Orpiada suffered swelling and blisters on her entire body after an allergic reaction
As Jenny Mariano Orpiada took her seat in the Dubai hospital room, she began to prepare for her checkup by gradually undressing, and with every layer that came off, she exposed a little more of the aftermath of the malady that had almost killed her.
There were large red patches all over her chest, where new skin had formed. Jigsaw puzzle piece like marks — brown on the edges and pink inside — covered her arms. Her lips were unnaturally puffy, uneven and brown. A closer look revealed missing nails on some of her fingers and toes. Giant dried blisters covered the entire heel of her feet. A painful looking two-cm blister was in the centre of her tongue with her eyebrows and lower eyelashes noticeably absent, although she had done a good job of penciling in her eyebrows with makeup.
“My top lashes will fall out too. And the rest of my nails, ” she said bringing her hand up to examine how many nails had been spared so far.
Pointing to her thighs she continued, “my legs are peeling now and have blisters, like the ones on my feet, all over them. I can show you if you like.” But a quick re-examination of her clothing which involved leggings that could not be rolled up and would have to taken off discouraged the idea.
“I have my vision back in my right eye but my left eye is still blurry, its like double vision,” she added.
A long white sheila, which she had wrapped around her head, neck and chest, and a surgical mask over her mouth had done well to cover the bulk of the evidence.
“The scarf and the mask are for protection, when I’m outside,” said Orpiada.
This appointment was a particularly important one for the 38-year-old Filipina. She had been taken off her immunosuppressive medication five days earlier and her dermatologist wanted to test her blood count levels. A positive result would provide reassurance that she is on the right track for recovery.
Orpiada’s health troubles began in January when she began to take the medication she was prescribed for a common health issue.
“I first went to a clinic (in Dubai) in December and saw a urologist because my stomach was really sticking out and bloated. They did some tests and said my uric acid level was high,” Orpiada explained.
She was told that normal uric acid levels for women should be between 2.6 – 6 mg/dL, her result showed an alarming 9.7mg/dL.
Orpiada was prescribed allopurinol, a common medication for treatment of high uric acid. However, a trip to the Philippines for Christmas made her forget to pack her medication.
Shortly after returning to Dubai from her vacation, Orpiada woke up one morning to find her left arm in pain and almost impossible to move.
She returned to the urologist and confessed that her vacation had prevented her from taking the prescribed medication. The doctor told her that her high uric acid was probably the cause of the pain in her arm, and after tests reconfirmed her uric acid levels had not changed, she was prescribed the same medication, allopurinol, as well as painkillers, Maxigesic Paracetamols, for the pain in her arm.
According to Orpiada, the doctor did not warn her about any possible side effects of the medication, on either visit.
“I took the medicine for about 10 days (allopurinol and Maxigesic Paracetamols) but then I noticed some lumps on my throat which were very painful,” she pointed to an area under her jaw, just below her ear, to show the exact spot.
Orpiada went back to the same clinic and saw an Ear, Nose and Throat (ENT) specialist. After a throat swab and an ultrasound of her neck, she was prescribed antibiotics, Cefpodoxime, plus more of the same painkillers and sent home.
She took the antibiotics for two days but woke up after the second day to find her face had swelled-up and her eyes hurt.
Orpiada stopped to scroll through the photographs on her phone and pulled out some selfies, which showed her with an unusually inflated face.
At this point she decided to stop taking her medication.
As the swelling on her face continued to worsen while she was at work, upon the advice of her colleagues she went back to the clinic where she was told she was having an allergic reaction. She was given antihistamines and sent home.
Exhausted and drowsy, Orpiada took a nap when she got home but woke up to find herself in an even poorer condition. Not only had the swelling on her face not reduced, she now had a red rash on her arms and there were blisters growing inside her mouth.
She returned to the clinic once more. This time she was given an antihistamine shot, an IV, and sent home again.
“I was in a lot of pain, specially my back. When I lay on my bed I could hear things popping on my back. But I forced myself to sleep,” she said.
Orpiada woke up in the morning to find the popping sounds were the painful blisters that now covered her entire back bursting. She also had a red rash on her entire body, giant blisters on her feet, a swollen face as well as blisters insider her mouth. “It was scary, I didn’t know what to do,” she recalled.
After consulting with a friend, she rushed to Medeor 24x7 hospital, in Dubai’s Embassy District area, accompanied by her sister. The doctor who examined Orpiada at the hospital, admitted her and called the specialist dermatologist urgently.
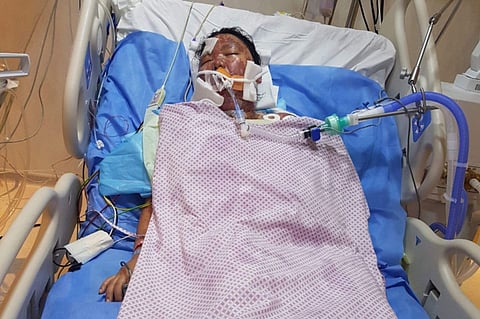
“She was not in a good condition. Because of the peeling blisters on her back and the bleeding blisters in her mouth, we immediately sent her to the ICU. We basically had to treat her like a burn victim,” said Dr Suresh Babu Rengasamy, Specialist Dermetoligist.
Orpiada was diagnosed with Toxic Epidermal Necrolysis (TEN), a potentially life threatening skin disorder that occurs in about one or two in a million people. TEN is believed to be caused by rare and unpredictable reaction to medication.
Dr Rengasamy said after examining Orpiada and the medication she had been taking, the medical team determined that she was most likely having a reaction to her uric acid medication.
However, as she took the medication with painkillers and antibiotics, it was difficult to confirm for certain. While skin rash is a possible side effect of allopurinol, Orpiada’s severe reaction is considered rare.
According to a 2012 study published by Arthritis Care and Research, an official journal of the American College of Rheumatology and the Association of Rheumatology Health Professionals, allopurinol is generally well tolerated. However, two to five per cent of patients may develop side effects including mild skin rash or gastrointestinal distress. It can cause severe hypersensitivity reactions characterised as a spectrum of clinical conditions ranging from a mild skin rash to life-threatening toxicity presenting as fever, hepatitis, vasculitis, eosinophilia, worsening renal function, and severe cutaneous adverse reactions (SCARs), including toxic epidermal necrolysis (TEN) and Stevens-Johnson syndrome (SJS).
Dr Rengasamy said Orpiada’s mortality rate was determined to be at a about a dangerous 30 per cent when they started treating her. He confirmed that TEN’s mortality rate varies depending on age, body surface area affected and blood parameters.
Her medical team suspected her TEN was caused by the allopurinol because Orpiada’s initial symptoms began before she started taking the antibiotics. However, the antibiotics she was prescribed also had swelling, severe blistering and red skin rash listed as possible side effects.
As Orpiada was being prepped in the ICU, she was still unaware of the seriousness of her condition and did not understand why the staff were making such a fuss over her. “They said they wanted to put a catheter on me, to pass my urine through it. I was telling them that I was fine and that I can go to the bathroom myself. I didn’t know that my blistering was getting worse,” she said.
She was so overwhelmed that she did not realise the reason they wanted to place a catheter on her was because she had developed blisters on and inside her genital area and doctors suspected that she could get worse and become immobile.
Her objections were ignored, a catheter was placed, along with an oxygen mask and she was given cyclosporine, a powerful immunosuppressant.
Dr Rengasamy explained that in simple terms, Orpiada’s immune system had suffered from many changes and caused her T lymphocytes, type of white cells, to attack her body. “The cyclosporine reduces the number of T lymphocytes, which we hoped would bring the attack under control,” he said.
But she continued to regress. “That evening, Orpiada said she was finding it hard to breathe. Her throat had severely swelled-up. She couldn’t even swallow her own saliva and was dribbling. She was deteriorating fast,” said Dr Rengasamy.
Concerned about her declining condition, the medical team decided they had to intubate her before the swelling in her throat got worse and blocked her airway completely. The ENT team was placed on standby to carry out a tracheostomy, just in case they were too late.
“We were lucky to perform the procedure when we did. A little later and we would not have succeeded and they would have had to cut into her throat. It was very difficult and we had to use a camera, but it worked,” said Dr Rengasamy.
“In her condition, we really did not want to have to open a hole in her throat too. It would have complicated her condition even more,” he added.
Orpiada was placed on a ventilator and sedated for the next eight days in an effort to keep her pain free. Concerned that the cyclosporine was not working fast enough, as Orpiada continued to develop blisters internally and externally, the medical team explored other options and agreed on a new approach.
Dr Rengasamy said they decided to take a chance and give Orpiada an Etanercept injection, a tumour necrosis factor-alpha (TNF-alpha) blocker. The drug suppresses the immune system by blocking the activity of TNF-alpha, a pro-inflammatory cytokine in the body. The medication is typically used to treat psoriasis, a type of skin disorder.
“It was very risky to do this because her body’s immunity was already low. Giving her this injection would lower her immunity even further and increase her chances of getting an infection, which could have caused further complications,” said Dr Rengasamy.
She was given the Dh7,000 etanercept shot, ordered specially for her, on her third day at the hospital and closely observed. The risk paid off, Orpiada did not develop any new rashes or blisters the next day. However, now not only the doctors had the task of treating her open injuries, they had to do it while protecting her from her weak immune system.
“Prevention of infection was the real challenge, we had to be extremely cautious. No one could enter Jenny’s room without the proper protection. We had to keep everything in her room aseptic,” said Dr Shahid Hussain, a General Practitioner and an ICU Registra at Medeor 24x7 Hospital, one of the ICU doctors who attended to Orpiada.
Hussain said every day, a team of eight, generally consisting of two doctors and six nurses, spent around two hours changing Orpiada’s dressings and cleaned her wounds.
“It was a very challenging procedure. Someone had to hold the breathing tube for two hours, we had to clean her wounds, change her dressings — very carefully — turn her, clean her, and change her sheets during this process,” said Dr Hussain.
Hussain explained that the sheer number of specialists who were involved in Orpiada’s case, which included a dermatologist, nutritionists, dieticians, physiotherapists, the hospital’s management, plastic surgeons, eye specialists, labs, nurses, and cleaners, called for extra vigilance. “A lot of coordination and arrangement was required,” he said.
Orpiada started to show signs of improvement but she was not out of danger yet.
The healing blisters on Orpiada’s eyelids were causing her eyes to close as she developed new skin on her eye margins, which if not attended to could cause her eyes to be shut permanently.
Nurses had to work around the clock to open her eyes regularly in order to prevent skin from forming over them. “Depending on the condition of her eyes, we had to open them every half hour to an hour,” said Dr Rengasamy. Which also meant no sleep for Orpiada.
The ulcers inside Orpiada’s eyes, on her cornea, caused her to have blurry and distorted vision and she said she developed an infection in her left eye. Under the care of an ophthalmologist, Orpiada was given cyclosporine eye drops, and she started to improve.
The team were faced with another serious issue when Orpiada’s back started to heal. “On the sixth day her back started to bleed. The skin was too fresh and the pressure of lying on her back was peeling the skin off,” said Dr Rengasamy.
After consulting with the team’s plastic surgeon, Dr Rengasamy said they worked hard to reduce her daily two-hour cleaning process and changed the type of dressing used on Orpiada’s back.
It worked. By the eighth day the bleeding had stopped. With her swellings reduced, blisters under control and a generally more stable condition, Orpiada was removed from the ventilator and sedation.
After 10 days in the ICU, Orpiada was finally out of danger and was transferred to the general ward where she would spend another 11 days receiving treatment and slowly gaining her strength before being released.
After her checkup with Dr Rengasamy, Orpiada’s blood count from her test came back normal. Although it is good news, she has a long way to go before she fully recovers. She has to follow a list of dos and don’ts for the foreseeable future, including avoiding direct contact with the sun for at least three months, wearing a mask when outside, avoiding crowded places, moisturising her skin regularly, and continue with her physiotherapy exercises to get her muscle strength back which she lost while she was bedridden and sedated.
Dr Rengasamy reassured her that her eyelashes and eyebrows will grow back in time and the scars will slowly fade away, although it may take up to a year.
Despite the horrific experience she endured and her long road ahead to a full recovery, Orpiada is surprisingly relaxed and upbeat. Her secret, she said, is her belief in God and love for her 13-year-old son, who lives with her husband in the Philippines.
“Through all this I kept praying to God to help me get well so I could see my son again. I couldn’t imagine not seeing him again, he is all I thought about. I am so grateful to be alive,” said an emotional Orpiada.
Sarvy Geranpayeh is a writer based in Dubai.



