Monkeypox vaccines: What to know about Imvamune, Imvanex, Jynneos, ACAM2000
Vaccines had been approved for monkeypox, but it's not just a matter of supply and demand
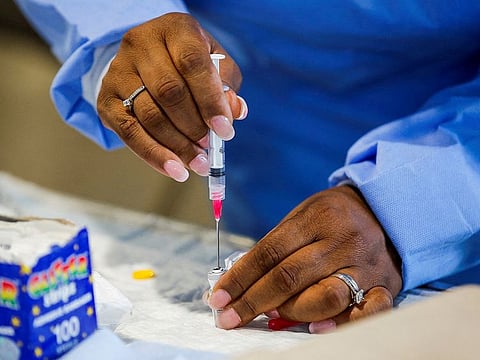
Highlights
- Vaccines approved for monkeypox are available, but in limited supply.
- Currently, there are at least 3 vaccines approved for use against monkeypox in the EU and US.
- Imvamune|Imvanex has been approved in the EU; Jynneos (another brand for Imvanex|Imvamune) has been approved in the US.
- Smallpox vaccine ACAM2000 has been approved by the FDA under an “expanded-access Investigational New Drug” protocol approval to allow its use for monkeypox.
Vaccines against monkeypox, repurposed from smallpox shots, exist and are being made available. Given the spike in monkeypox cases globally, starting in Europe in May 2022, demand for vaccines has shot up.
Last week, the WHO declared the monkeypox outbreak a global health emergency. Though less severe than smallpox, monkeypox can cause deaths (up to 10% for the Central African "clade"). Fatalities had now been reported outside Africa (where it is deemed "endemic"): one in Brazil, two in Spain and one was confirmed in in India on Monday.
Vaccination is one of the best tools available to help curb the outbreak, in addition to following recommended protocols.
MONKEYPOX CASES SO FAR
Confirmed monkeypox infections jumped 74-fold — from just 226 cases in 22 countries (as of May 27) to more than 16,800 cases in 74 countries as of Friday (July 22). Cases rose to 22,485 as of July 29, 2022 in 79 locations (of which 72 have not historically reported monkeypox infections), according to the US Centres for Disease Control and Prevention. US cases have climbed from just 40 confirmed infections on June 8, 2022 to 5,189 on July 29, 2022.
How serious is monkeypox infection?
Monkeypox virus is not new (first discovered in 1958), with repeated outbreaks in West and Central African countries. It triggers fever, headache, muscle aches, backache, swollen lymph nodes, a general feeling of discomfort, exhaustion, and severe rash. Studies of monkeypox in Central Africa showed that the disease killed up to 11% of people infected.
The main upside with vaccines is that most people who get the smallpox or monkeypox vaccine have only minor reactions, like mild fever, tiredness, swollen glands, and redness and itching at vaccination site. CDC noted that these vaccines do have more risks, too. Some can be serious.
What we know so far:
What are the approved monkeypox shots?
Currently, the smallpox vaccines also approved for monkeypox are: Imvanex|Imvamune, Jynneos and ACAM2000.
The European Medicines Agency (EMA), EU’s drug watchdog, recently approved (July 22, 2022) Imvanex|Imvamune, valid in all of EU 27 member-states, Iceland, Liechtenstein, and Norway.
In the US, the 2 vaccines approved for monkeypox are: Jynneos (also known by their European brand names Imvanex|Imvamune) and ACAM2000.
On July 27, 2022 FDA stated that ACAM2000 was granted an expanded access Investigational New Drug (EA-IND) protocol to allow its use for monkeypox.
How does Imvanex | Imvamune work?
It contains an attenuated (weakened) form of the vaccinia virus.
Imvanex is derived from replication-competent dermal vaccinia strain Ankara “attenuated” after >570 continuous passages in primary chicken embryo fibroblasts that has undergone 6 rounds of “plaque purification” and is propagated in serum-free conditions, according to the WHO.
Imvanex|Imvamune is given by injection under the skin, usually in the upper arm. People who have not been previously vaccinated against smallpox, monkeypox or the disease caused by the vaccinia virus should receive the recommended two 0.5-ml doses, with second dose given at least 28 days after the first.
Side effects: What is the safety profile of Imvanex | Imvamune?
The WHO has cited safety summary data from completed and ongoing clinical trials in which more than 7,600 individuals received the vaccine. Those who were vaccinated included:
> Vaccinia-naive and experienced populations
> HIV positive persons
> Persons with atopic dermatitis.
The majority of events were local and systemic reactions, were “mild” to "moderate” and resolved rapidly without intervention. The vaccine was well tolerated with no clinically-relevant differences between the populations studied, the WHO vaccine experts committee reported.
No confirmed case of myopericarditis or any other cardiac inflammatory event in any Imvanex/Imvamune (Phase 3) clinical trial was observed.
The shot is manufactured by Danish drugmaker Bavarian Nordic.
How does Jynneos vaccine work? What are the known side effects?
Jynneos, approved in the US, is another brand of the Imvanex|Imvamune vaccine. Known side effects and adverse events associated with Jynneos reported in the US include:
> Injection site reactions (pain, redness, swelling, a hard lump, and itching)
>Muscle pain
>Headache
>Fatigue
>Nausea.
The FDA reported no vaccine-related foetal malformations or variations and adverse effects on female fertility or pre-weaning development in these studies.
FDA has also approved Jynneos vaccine in adults 18 years of age and older at higher risk of smallpox or monkeypox infection.
Jynneos is administered as two subcutaneous injections four weeks apart. People who receive Jynneos are considered vaccinated 2 weeks after they receive the second dose of the vaccine.
On November 3, 2021, the FDA voted to recommend Jynneos as a pre-exposure prophylaxis (preventive shot) for monkeypox.
Past data from Africa suggests that the smallpox vaccine is at least 85% effective in preventing monkeypox. The effectiveness of Jynneos against monkeypox was concluded after a clinical study on the “immunogenicity” of Jynneosand efficacy data from animal studies.
How does ACAM2000 work?
The vaccine is made from a virus called vaccinia, a "pox"-type virus related to smallpox but causes milder disease. ACAM2000's biggest advantage: It cannot cause smallpox, as it does not contain the smallpox virus. In Phase III trials, ACAM2000 reported an 84% efficacy in inducing neutralising antibodies.
Rather it has the "live" vaccinia virus. For this reason, attentively caring for the vaccination site is important to prevent the virus from spreading from the vaccination site to other parts of the body, or to other people.
On the other hand, the FDA recommends JYNNEOS pre-exposure prophylaxis as an alternative to ACAM2000 for certain persons at risk for exposure to orthopoxviruses.
How is ACAM2000 administered?
ACAM2000 is administered using a two-pronged stainless steel (or bifurcated) needle is dipped into the vaccine solution and the skin is pricked several times in the upper arm with a droplet of the vaccine. The virus begins growing at the injection site causing a localised infection or "pock" to form, FDA explained.
A red, itchy sore spot at the site of the vaccination within 3-4 days is an indicator that the vaccination was successful — that is, there is "a take."
After a blister develops at the vaccination site, and then dries up. A scab is formed that then falls off in the third week, leaving a small scar.
The vaccine helps stimulates a person's immune system to develop antibodies and cells in the blood and elsewhere that can then help the body fight off a real smallpox infection if exposure to smallpox ever occurs.
What is the prescribed ACAM2000 dosage?
ACAM2000 is reconstituted by addition of 0.3 mL of diluent to the vial containing lyophilised (freeze-dried) powder vaccine, according to the FDA. After reconstitution, each vial has approximately 100 doses of 0.0025 mL of live vaccinia virus, containing 2.5 – 12.5 x 105 plaque-forming units.
The shot using a bifurcated needle must be administered only by vaccine providers trained to safely and effectively administer the vaccine via the percutaneous route.
Who can receive|not receive ACAM2000?
ACAM2000 is not harmful to healthy people, though it can cause serious illness in people under the following categories:
> Those who are severely immunocompromised (including people with advanced or untreated HIV)
> Pregnant women
> People with eczema
> Infants.
WHO reported that serious adverse effects from clinical trials with ACAM2000 include myopericarditis and cardiomyopathy. The updated safety information for ACAM2000, however, did not reveal any new areas of concern after administration to approximately 1 million people.
ACAM2000 needs special training for vaccinators as it is inoculated into the skin with a two-pronged needle through a series of tiny jabs at the skin — enough to draw a droplet of blood.
> Inoculation site signs and symptoms
> Lymphadenitis
> Constitutional symptoms, such as malaise, fatigue, fever, myalgia, and headache.
In revaccinated persons, these adverse events tend to be less frequent than persons receiving the vaccine for the first time.
Do these vaccines really work?
According to the CDC, when properly administered before an exposure, vaccines are effective at protecting people against monkeypox.
Because Monkeypox virus is closely related to the virus that causes smallpox, the smallpox vaccine can protect people from getting monkeypox.
Can I get the jab after exposure?
Vaccination is recommended for persons exposed to monkeypox virus and who have not received the smallpox vaccine within the last 3 years.

_resources1_16a3107bd6c_medium.jpg?w=320&auto=format%2Ccompress&fit=max)





