Anyone can be at risk of Long COVID-19
Coronavirus hits the old hardest, but the healthy can be impacted longest
Before he had COVID-19, Brendan Delaney, the 57-year-old chair of medical informatics and decision making at Imperial College, could cycle 150 miles in a day. COVIDchanged that, but not because he had a severe case of the disease.
Delaney never got seriously ill from the virus. Like many healthy people, he figured his symptoms, a mild fever and a cough, would pass soon enough. Instead, he experienced debilitating aftereffects, such as fatigue and breathlessness, which many are now calling Long COVID. Seven months later, he is still not back to normal. He can’t imagine getting back on a bike and says that if he pushes himself too hard, he ends up in bed with a fever for a couple of days. He considers himself lucky that he’s able to work. Many other Long COVID sufferers cannot.
As a second wave of infections grows, so it follows that the number of Long COVID cases is bound to increase. Although this clearly has implications for public health and the economy, it has been almost nowhere in the broader policy debate.
That narrative has focused largely on minimising deaths and hospitalisation. But most Long COVID patients weren’t hospitalised and didn’t have pre-existing conditions. This should throw some cold water on the idea of dispensing with restrictions and allowing immunity to build up among the young while shielding the vulnerable “- an approach that has won more adherents as lockdown fatigue set in. Going in this direction would be far more costly than many perhaps realise.
“We need to control this virus not because of the risk that granny may catch it and die, or your uncle may end up in ICU, but because fit, healthy people without any comorbid conditions who are young can end up having their lives wrecked,” Delaney says during a conversation over Zoom.
We know from experience with other viruses “- from the 2003 SARS outbreak to Ebola, MERS and glandular fever (caused by the Epstein-Barr virus) “- that effects can be long lasting. It’s similar with today’s coronavirus. Studies suggest a significant number of COVID-19 patients will have symptoms that linger and can affect different organs and systems.
Conventional medicine, however, doesn’t have a good record on responding to conditions where the cause can’t easily be isolated, which is the case with Long COVID. For years, sufferers of Chronic Fatigue Syndrome, Lyme disease, Endometriosis and other conditions often fought lonely battles for recognition and medical care. The most reported symptoms of Long Covid sound like they could be any number of illnesses: extreme fatigue, breathlessness, heart palpitations, gastrointestinal problems, joint pain and problems with memory and focus. A cross-party UK parliamentary group identified 16 common symptoms, but the full list is much longer. In many cases, sufferers never had a Covid test (they weren’t widely available) and blood tests and scans don’t reveal any major abnormalities.
The good news is that there are too many cases like Delaney’s to ignore, and so recognition and media attention is coming faster than it has in other cases. The UK is ahead in some ways. Health Secretary Matt Hancock, a slim 42-year-old who had COVID-19 back in March and recovered quickly, has spoken publicly about the long-term effects. The National Health Service created a support website and put aside 10 million pounds ($13 million) to set up a network of Long COVID clinics in England. An official definition, expected this month from Britain’s standards-setting National Institute for Health and Care Excellence (NICE), will give a better indication on how seriously the condition is being taken.
Even so, existing UK measures will be small beer if the virus continues to spread and Long COVID cases mount. Nailing down exact numbers isn’t easy, but one in 10 users of the COVID Symptom Study app, used by more than 4.3 million UK participants, reported symptoms persisting for more than three weeks after infection. Some 60,000 reported symptoms that lasted more than three months. Delaney says this may be an underestimation since symptom trackers are used largely during the acute stage of the virus.
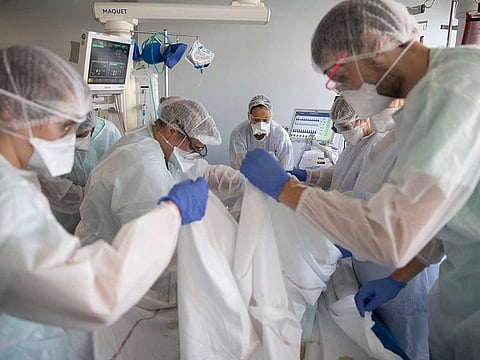
This is already posing problems for health professionals. Shortages of personal protective equipment and inadequate guidance early in the pandemic put medical staff at greater risk of contracting the virus. When the British Medical Association asked 5,650 doctors about their experience, almost 30% of those who’d had COVID were left with physical fatigue and shortness of breath; 18% described some kind of cognitive impairment. About a fifth had taken sick leave to deal with the symptoms. Delaney says he knows of two doctors with Long COVID symptoms who lost their jobs because they were unable to return to full-time work. (In France, a recent decree limits disability claims by health care workers to those who required oxygen to treat the virus.)
Increasing infection rates have ushered in fierce debates over the relative costs, benefits and ethical considerations of various lockdown measures. Long COVID may alter that calculus further, depending on the impact on household income and productivity. A 2004 US study using cost-of-illness analysis to estimate the impact of Chronic Fatigue Syndrome (which has similar symptoms to Long COVID) concluded that it probably led to a 37% decline in annual household productivity and a 54% reduction in labour force productivity among sufferers, with a total annual lost value of $9.1 billion a year.
How the Long COVID costs stack up will depend on various things including prevalence, duration of symptoms and the degree of incapacity. It does seem that symptoms slowly get better over time, though it’s too early for a tally of long-term effects such as fibrosis of the lungs or compromised immune systems. Although more research is needed, the existing picture warns against a view that divides the population into neat high- and low-risk categories. “Whether or not you think you are at risk of ICU admissions, anyone can be at risk of Long COVID,” Delaney says.
That’s a sobering thought, but it may at least encourage a little more solidarity as we figure out how best to control a second pandemic wave.
Therese Raphael is a columnist. She was editorial page editor of the Wall Street Journal Europe
Bloomberg







