Why black fungus aggravates COVID-19 crisis in India
White fungus and yellow fungus are also ravaging people with poor immunity and diabetes
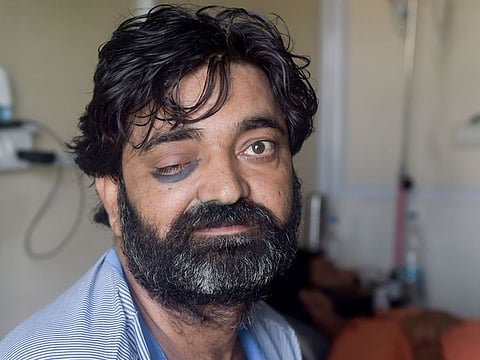
Black fungus. White fungus. Yellow fungus. Kunwar Singh suffered from these three types of fungus before he died in a Ghaziabad hospital near New Delhi in May. Singh, 59, had been recovering from COVID-19, but fungal infections proved fatal.
Singh, a lawyer, is believed to the first patient to suffer from the three types of fungus, Indian media reported. “The yellow fungus, besides white and black fungus, was detected during an endoscopy,” the Press Trust of India quoted Dr Brajpal Singh Tyagi, an ENT surgeon, as saying.
Black fungus is mucormycosis, while white and yellow fungi refer to aspergillosis, candidiasis and cryptococcosis. These invasive fungal infections affect people with compromised immune systems. Misuse of steroids and antibiotics can impair human immune response, and this is cited as a primary cause of increased fatal fungal infections in India.
Around 12,000 cases of mucormycosis have been reported from India, mostly patients recovering from COVID-19. Severe infections are rare, and fatality rates are generally very low, which is why medical experts are stumped by the fungus-related deaths in India. More than 300 deaths have been recorded so far.
Fungal diseases kill more than 1.5 million people and affect over a billion more worldwide annually. Most of these deaths are avoidable if public health authorities paid more attention, a paper in the Journal of Fungi said.
Why is India grappling with a high rate of fungal infections?
Steroids and antibiotics are used for COVID-19 treatment in India. That coupled with a high number of diabetics in the country have made fungal infections fatal. Fungal infections can be treated, but a shortage of medicines like Amphotericin-B has made a bad situation worse.
Writing in The Conversation, Rajib Dasgupta, chairperson of Centre of Social Medicine and Community Health at Jawaharlal Nehru University, said: “The [Indian] government’s own guidelines for steroid use are so much higher than in other countries, there should be analysis into whether this may be contributing to the significant rise in fungal infections.”
Self-medication is said to be another cause of fungal infections as medicines are freely available in India and controlled drugs can be procured with money and the right connections, experts say. Since hospitals are overwhelmed, many people are self-medicating. That leads to improper dosage and poor attempts to taper off the medication resulting in impaired immunity.
Using oxygen therapy at home without proper hygiene could also lead to fungal infections, experts add.
What’s fungus?
Fungus belongs to about 144,000 known species of tiny organisms of the plant kingdom Fungi, which includes yeasts, rusts, smuts, mildews, molds, and mushrooms, according to Encyclopaedia Britannica. Other organisms, like slime moulds and water moulds), are not part of kingdom Fungi but are referred to as fungi.
Some fungi, like mushrooms, are edible, but others like aspergillus are dangerous and could lead to life-threatening diseases.
What is a fungal infection?
Mycosis is the medical term for a fungal infection. Some fungi are capable of causing diseases under specific conditions like compromised immunity. These are known as opportunistic infections. Generally, our bodies can keep fungal infections at bay, but conditions like diabetes and poor immune response can lead to complications.
Fungal infections are most likely to affect your skin, nails, or lungs. Fungi can also penetrate your skin, affect your organs, and cause a body-wide systemic infection, a report in Healthline said. Some common types of fungal infections include: athlete’s foot, jock itch, ringworm, yeast infection and onychomycosis, or fungal infection of the nail
What’s black fungus or mucormycosis?
Mucormycosis is a rare fungal infection caused by a group of moulds called mucormycetes (mucor mould) found in the environment. Mucor mould is commonly found in soil, air and even in the nose and mucus of humans. Previously called zygomycosis, mucormycosis mainly affects the sinuses or the lungs of people with reduced immunity. Inhalation of fungal spores can lead to the disease, which can also occur on the skin after a cut, burn, or other skin injuries.
The condition is relatively rare; it affects only one in 1 million people, but its mortality rate is 50 per cent.
“Fungal spores are everywhere, but we are pretty efficient at clearing them from our lungs. But COVID damages the lung. So then you have a double whammy: reduced capacity to naturally clear the spores and reduced immune response as a result of steroids,” the Scientific American quoted Arturo Casadevall, a molecular microbiologist at the Johns Hopkins Bloomberg School of Public Health in Maryland, US.
What are the common symptoms of black fungus?
Severe headache with pain over the forehead, temple or the top of the head is a common symptom. Others include toothache in the upper jaw, pain in eyes, nose block, blood in nasal discharge. Double vision, fever, seizures, stroke or paralysis are among the severe symptoms.
What are the different kinds of black fungus and their symptoms?
Different types of black fungus are named after the site of growth in the human body, according to the US Centres for Disease Control and Prevention. When it affects the sinus and the brain, it’s called rhinocerebral mucormycosis. When the fungus grows in the lung, it’s pulmonary mucormycosis; gastrointestinal mucormycosis refers to growth in the gut and intestines; blister-like growth on the skin is cutaneous mucormycosis, and disseminated mucormycosis occurs in people suffering from other medical conditions.
The infection spreads through the bloodstream to another part of the body. The infection most commonly affects the brain and can affect other organs such as the spleen, heart, and skin.
How does black fungus spread?
Mucormycosis is not contagious, so it can’t spread by oxygenation, humidifier, and water. It does not spread from one person to another. The fungi spores that spread through the air enter the respiratory tract and can affect facial structures.
What’s the treatment?
If mucormycosis is suspected, and a doctor will call for CT or MRI scans. An endoscopy may also be used to confirm the diagnosis, and samples will be sent for fungal studies.
What’s the surgical intervention for fungal infections?
Surgery to contain a relatively lethal disease that may involve removing facial bone and adjacent non-bony structures. Some doctors in India are forced to remove people’s eyes and jaw bones to stop the spread of the infection before it reaches the brains. These surgeries save patients, but leave them disfigured permanently.
Anti-fungal injections will follow this for at least a week. Sometimes, treatment is protracted and might warrant repeated removal of dead, damaged, or infected tissue and more extended hospital stay; a lot depends on patient response to treatment.
How deadly is the fungal infection?
Mucormycosis has an overall mortality rate of 50 per cent.
Why is mucormycosis killing COVID patients?
Steroids are suitable for treating lung inflammation and are useful in stopping the damage inflicted by a cytokine storm (when the body’s immune system goes into overdrive to fight off coronavirus). But steroids also reduce immunity and push up blood sugar levels in COVID-19 patients with and without diabetes. Reduced immunity could be triggering these cases of mucormycosis, doctors say.
Why are people with diabetes more at risk of black fungus infection?
In some cases, steroids wreak havoc on the sugar levels of COVID-19 patients, which makes them vulnerable to black fungus infection. “What is more worrying is that the use of steroids for treating certain cases of COVID-19 would shoot up sugar levels; this coupled with lack of physical activity puts diabetic people at a higher risk of catching the black fungal infection,” Dr Sweta Budyal, senior consultant endocrinologist, Fortis Hospital, Mulund, Mumbai, told the Indian Express.
According to a research paper in the Journal of Fungi, 94 per cent of patients with diabetes recovering from COVID-19 suffered from fungal infections.
More than 10 per cent of the adult population, 77 million people, in India suffer from diabetes, according to the 2019 International Diabetes Foundation Atlas.
How can you prevent this infection?
Since poorly controlled diabetes plays a significant part in fungal infections, good glycemic control during the management of COVID-19 patients is required.
One way to reduce fungal infections is to ensure that COVID-19 patients are administered the correct dose and duration of steroids during treatment, and after recovery, Dr Budyal says. It is also important for people with diabetes, cancer, kidney and liver diseases, and organ transplant patients to check their glucose levels from time to time, she adds.
Dr Budyal recommends that patients, who have recovered from COVID-19, should be advised about the early signs of mucormycosis (facial pain, nasal blockage and excessive discharge, chest pain, respiratory issues).
Which countries have black fungus?
Mucormycosis has been reported from at least 38 countries before the COVID-19 pandemic. According to the Leading International Fungal Education portal, the highest rates of black fungus cases were in India and Pakistan with around 140 cases per million annually.
What is white fungus?
White fungus or candidiasis is an infection caused by a type of yeast known as Candida. Commonly called thrush in some countries, candidiasis manifests as white patches on the tongue, lips, gums, the roof of the mouth, inner cheeks or throat. So patients may feel sore in the mouth or experience pain while swallowing. Candida is found on the skin and in the mouth, throat, gut, and genitals.
Who are at risk of white fungus infection?
People with diabetes and patients treated with steroids and antibiotics are vulnerable to candidiasis (white fungus). Other contributing factors include the use of dentures and smoking. Cancer and HIV patients too are at a high risk of being infected.
Proper sanitation and good hygiene are essential to prevent fungal infection since the spores thrive on damp surfaces. Most cases in India have been reported from Bihar, while isolated cases were found in Delhi and other places.
White fungus or black fungus, which is more dangerous?
White fungus can be more dangerous than black fungus if Candida enters the bloodstream (usually through poorly sterilised medical equipment). It can travel through the blood to the heart, brain and eyes, leading to a life-threatening infection. A weakened immune system and diabetes increase the risk as with other fungal infections.
What’s yellow fungus?
Yellow fungus, or mucor septicus, is an infection generally found only in reptiles. Of late, these rare fungal infections are afflicting people who have undergone steroid treatments for COVID-19.
Like other fungal infections, the yellow fungus spreads through contaminated areas or when a person inhales moulds (mycometes) found in the environment.
How different is the yellow fungus infection?
The yellow fungus infection attacks the body’s internal organs, thereby disrupting the body functions. Dr Tyagi, an ENT specialist in Ghaziabad, told ANI news agency that since yellow fungus begins to grow internally, it’s difficult to notice the symptoms, leading to deaths.
What are the symptoms of yellow fungus infection?
Lethargy, weight loss, poor appetite are common symptoms. If the infection is not treated, symptoms could become more severe, including pus leaks and slow healing of wounds, sunken eyes, organ failure, and necrosis (when cells in tissue die prematurely), according to Dr. Tyagi.
Is it more dangerous than black and white fungus?
Yellow fungus can be treated if the infection is detected early. Delay in detection makes it tough to cure than black and white fungal infections. Untreated infections can result in organ failure.
What causes yellow fungus?
High levels of humidity promote the growth of fungus. So poor hygiene is a leading cause. According to medical experts, other reasons could be prolonged and irrational use of steroids, uncontrolled diabetes, compromised immunity, and comorbidities (underlying health conditions).
How does it spread?
Fungal infections are generally not contagious, but they can prove fatal for people with compromised immunity. A person is infected when he/she inhales moulds found in the environment. Yellow fungus infections can spread due to high levels of humidity, and old and contaminated food can be good breeding grounds for the mould. Poor hygiene and unsanitary conditions remain to be the prime reasons for infection.
What is the treatment for yellow fungus?
Like black fungus, yellow fungus is also treated with anti-fungal drug Amphotericin B. The medicine has to be administered under medical supervision only, so patients have to hospitalised quickly and their symptoms monitored.